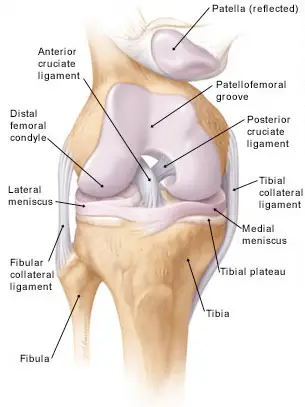
The knee is one of the strongest joint in your body. It is made up of the lower end of thighbone, the upper end of the shinbone, and the patella (kneecap). The ends where these bones touch each other are covered with a smooth covering called articular cartilage. This covering protects and cushions the bones as the knee moves through the entire range of motion.
The knee also contains two wedge-shaped shock absorbing gel pads called meniscus between your thighbone and shinbone. These tough and rubbery gel pads help cushion the joint and keep it stable. The knee joint also contains a thin lining of fluid secreting tissue called the synovial membrane which releases fluid that lubricates the cartilage and reduces friction.
Bones are connected to one another by ligaments. There are four primary ligaments in your knee. They act like strong pillars to hold the bones together and keep your knee stable.
Collateral Ligaments - These are found on the sides of your knee. The medial collateral ligament is on the inside and the lateral collateral ligament is on the outside. They control the sideways motion of your knee and brace it against unusual sideway movement of the knee joint.
Cruciate Ligaments - These are found inside your knee joint. They cross each other to form an "X" with the anterior cruciate ligament in front and the posterior cruciate ligament in back. The cruciate ligaments control the abnormal back and forth motion of your knee.
The anterior cruciate ligament (ACL) prevents forward motion of the leg bone (tibia) while the posterior cruciate ligament prevents the backward movement of the tibia. You can partially or completely tear the ligament(s) when the knee is injured along with other structures in the knee joint.
The collateral ligaments are firmly attached to the lower end of the femur (thigh bone) and the upper end of the tibia and fibula (lower leg bones). The ligaments hold the two bones together and prevent side to side motion.
Injured ligaments are considered "sprains" and are graded on a severity scale. About half of all injuries to the anterior cruciate ligament occur along with damage to other structures in the knee, such as articular cartilage, meniscus, or other ligaments
Grade 1 Sprain
The ligament has been slightly stretched, but is able to help keep the knee joint stable.
Grade 2 Sprain
The ligament has been stretched to the point where it becomes loose. This is often referred to as a partial tear of the ligament.
Grade 3 Sprain
The ligament has been split into two pieces and the knee joint is unstable.
The ACL can be injured either by contact injury such as road traffic accidents or direct impact on the knee or by non-contact injury such as twisting movements of the knee.
Contact-related ACL injuries usually occur from a direct blow causing hyperextension or when the knee is forced inwards towards the other leg. This is often seen in rugby when a player's foot is planted and an opponent strikes him on the outside or front of that thigh.
Non-contact anterior cruciate ligament (ACL) injuries typically occur when a person is running or jumping and then suddenly slows and changes direction (eg, cutting) or pivots in a way that involves rotating or bending the knee sideways. Women appear to be at a higher risk of non-contact ACL injuries than men, although the exact reason for this is not clear
ACL injuries most commonly occur during activities such as downhill skiing, gymnastics, tennis, rugby, soccer, and basketball which involve changing direction rapidly, stopping suddenly or direct injury to the knee or slowing down while running/landing from a jump incorrectly.
Some of the common symptoms of an ACL injury are
A physician may suspect an ACL injury by correlating your medical history with a thorough clinical examination of the knee. However, most patients visit the clinic immediately after the injury and hence it is not always possible to maneuver the injured knee joint for examination in the acute phase. It is therefore advisable to undergo imaging studies which will confirm exact nature and extent of the knee injury. Imaging studies also help to reveal silent injuries to other structures of the knee joint concomitantly injured along with the ACL. The imaging test include X-rays/Magnetic resonance imaging (MRI) scan.
Anterior cruciate ligament (ACL) injuries are treated either with surgery and post-surgical rehabilitation or with a non-surgical rehabilitation program.
The decision to have surgery is based upon several factors, including your age, how active you are, and whether you have other knee injuries.
You may choose to have surgery if you are
Most programs require daily strengthening and stretching exercises and one or more weekly visits with a physical therapist for the first three to six months after surgery. Failure to follow this program could increase the risk of re-injury, allow scar tissue to develop, and lead to limited movement of the knee.
You can choose to treat your Anterior Cruciate Ligament non-operatively if you
If you do not have surgery to reconstruct your ACL, you may be at an increased risk of future knee problems, including chronic pain, a decreased level of activity, and injury to other parts of the knee (the meniscus). However, surgery is also not a "quick fix," as it involves a recovery period and requires committing to rehabilitation program.
The time between an ACL injury and surgical reconstruction depends upon how quickly the person recovers from the acute phase of the knee injury, but is often at least two to four weeks from the date of injury.
Surgery is not usually performed immediately after an ACL injury because this could cause excessive scar tissue (arthrofibrosis) to develop, which would limit knee motion. In most cases, surgery is delayed until
the swelling has resolved and the person is able to bend and straighten the knee without difficulty. Using ice packs and elevating the knee above the chest can help to reduce swelling.
During the time between the injury and the surgery, many surgeons recommend a "pre-habilitation" exercise program to help reduce pain and swelling, improve range of motion (the ability to flex and extend the knee), and increase strength in the muscles of the thigh, knee, and hip. Walking, bike riding, and swimming (with light kicks and no breast stroke) can be continued, although other sports should be avoided.
After the ACL is torn, it is not possible to repair the ligament. This is due to several factors, including a damaged blood supply to the ligament (blood vessels damaged during injury) and cells inside the synovial fluid (normal fluid in the knee), that prevent healing. Research is underway to determine how to repair the ligament, but the only proven way to repair the ACL currently is to reconstruct it.
During the surgical reconstruction most people are given regional anesthesia (anesthetizing only the surgical part) and sedation prevent pain. The surgery itself usually takes less than two hours.
To reconstruct the torn ligament, a piece of healthy tendon, called an autograft, is removed or "harvested" from another area in the leg. There are several common autograft sites in the body, including the patellar tendon, hamstring tendon, or rarely the quadriceps tendon. Another option is to use a tendon from a deceased donor, called an allograft. No one type of graft has been proven to be better than another. Thus, the type of graft that is used depends upon the surgeon's preference and experience.
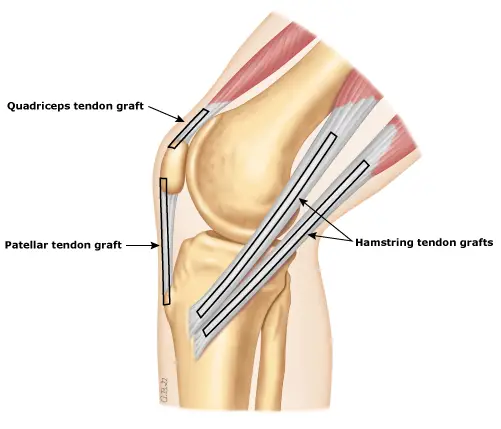
Hamstring autograft – If using a hamstring autograft, there are no extra incisions needed and the pain at the harvest site is usually less than that seen with a patellar autograft. Hamstring strength usually returns to normal within three to six months
Patellar autograft – When harvesting a patellar autograft, an extra incision is made in the skin to remove a strip of tendon with a piece of bone at each end. The graft site usually heals quickly and regains normal strength. Some people have soreness in this area for several months after surgery, especially if pressure is applied to the area (eg, while kneeling).
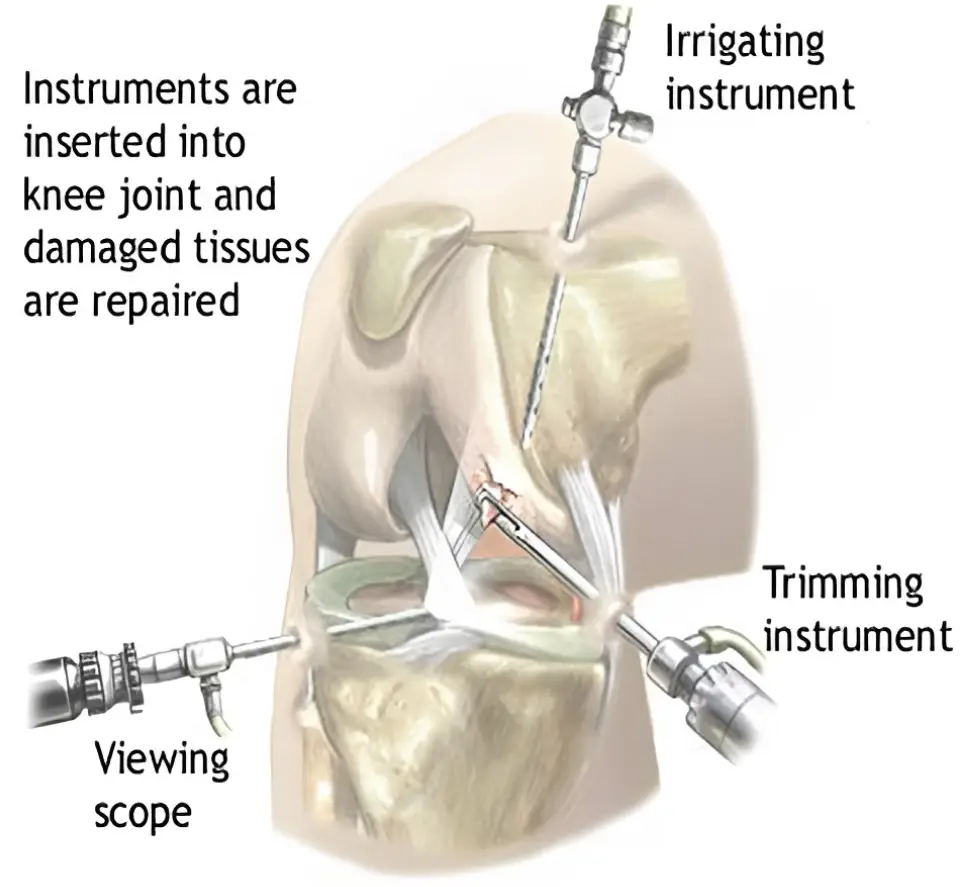
The torn ACL is removed and replaced with the graft using a narrow telescope-like device, called an arthroscope. The scope contains a camera and light source, and can be inserted into the knee joint through a small skin incision. Instruments are inserted into the knee joint through other small incisions, allowing the physician to place the graft with precision. After the graft is secured with implant, the knee is wrapped with sterile dressings and an immobilizer is placed around the knee.
What are the possible complications of ACL surgery
Most people do well after ACL reconstruction and have no major complications. However, complications rarely occur during surgery or during the rehabilitation period. The most common complications include:
ACL reconstruction is major surgery and recovery is challenging if you are not aware of the whole process. Having realistic expectations can be helpful in both making the decision to have surgery and preparing for the recovery period.
During the first few days, the goal is to control swelling and pain. Elevating your knee above your chest and applying ice are the best ways to do this. Most people use crutches to assist with walking for the first week or so after surgery, although you will likely be encouraged to begin bearing weight on the affected leg as soon as possible. (If your surgery was more extensive, your surgeon may recommend delaying weight bearing for a longer period.)
You will probably need to wear a brace that keeps your leg straight for few weeks after surgery. This brace protects your knee, but many surgeons recommend removing it to do gentle range-of-motion exercises (with a CPM machine) beginning about three to five days after surgery. Stretching and strengthening exercises can usually begin a few days after surgery. Your surgeon will give you a detailed plan for the rehabilitation protocol to be followed upon after discharge from the hospital. You are strongly advised to consult a physiotherapist to initiate the rehabilitation protocol.
It's important to keep in mind that everyone heals differently. While your surgeon can give you a general idea of how long your recovery will take and how you will feel at each stage, this can vary. It may help to keep in mind that even though the recovery can be challenging, especially in the early weeks, you will likely be back to most of your normal activities after about six months. Depending on your sport(s), it may take a bit longer to return to full participation.